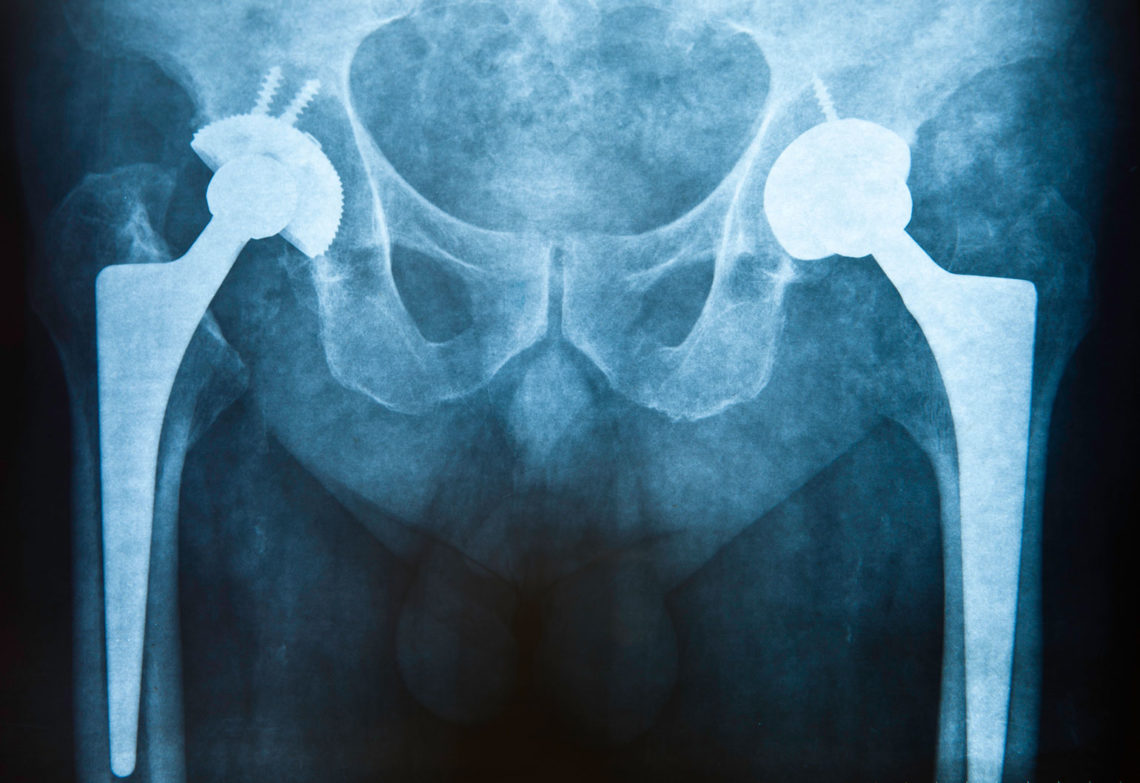
Australia’s ageing and active population means the number of orthopaedic implants is on the rise. A new plasma coating could lead to longer implant lifespans by ‘hiding’ it from the body.
Orthopaedic implants like knee or hip replacements can be life changing, relieving pain and giving recipients greater freedom to live and move as they please. But while surgeries are fairly routine these days, they still come with complications. One is that the body might reject the implant, and another is the risk of infection.
A team of engineers, physicists, materials experts and medical professionals has worked to develop a new plasma coating for bone implants to address these concerns. The research is a collaboration between the University of Sydney’s School of Aerospace, Mechanic and Mechatronic Engineering, School of Physics and School of Civil Engineering, the Heart Research Institute and the University Medical Centre Utrecht in the Netherlands, and received additional financial support from the Australian Research Council.
Their work, published in Applied Materials Today, investigated the interaction of plasma-generated coatings with human-derived stem cells. It found that the new coating could enhance the functionality of bone-producing cells, allowing an implant to bind firmly to a host bone.
“Our latest research presents great promise for the creation of a new class of robust, bio-active surfaces for orthopaedic implants,” said lead author and plasma surface engineering expert Dr Behnam Akhavan, from the University of Sydney.
In plain sight
As Australians’ average age rises, so does the incidence of joint replacements – totalling about 90,000 devices per year at a cost of almost $1 billion.
And while surgical techniques and post-operative care have improved, implants can fail due to infection or poor integration with the surrounding bone tissue.
While the research team previously developed an antimicrobial coating, they found firm bone bonding was also needed to prevent loosening, and thus avoid costly and risky revision surgeries.
The new plasma coating is a mixture of argon, nitrogen and acetylene gas, and bone-signalling molecules are applied to encourage stem cells to produce bone, addressing the importance of bone integration.
“The implants have been surface engineered using the plasma technology and will be overgrown with bone-producing cells once implanted in the body, allowing them to firmly attach to bone tissue,” Akhavan said.
Akhavan added that the bioactive molecule coating “hides the metallic implant from the body, so it is treated as a biological structure rather than an invasion”.
“Rapid implant integration reduces the chance of an implant loosening and failing, therefore eliminating the need for revision surgeries,” he said.
“The mechanically strong coating can remain on the implant surface for long durations, even if it is scratched during surgery.”
Mimicking the body
Team member Professor Marcela Bilek, who works within the University of Sydney’s Applied Physics and Engineering department, said the application of plasma coatings on implantable devices is a step closer to creating materials that perfectly mimic the surrounding tissue.
“This coating is fully organic and is a significant advancement because it robustly adheres to titanium implants, while presenting strongly attached biological signalling molecules that guide tissue formation at its interface with the body,” she said.
Initial testing of the coating showed promising results, Akhavan said, and has led to in-vivo testing in the Netherlands.